AI in Pharmacovigilance: The Dawn of a Data-Driven Safety Revolution
Dr. S. Neelufar Shama, Professor & Head, Department of Pharmacognosy, Scient Institute of Pharmacy
Pharmacovigilance is the cornerstone of drug safety monitoring. It also faces challenges like vast data volumes, diverse information sources and need for rapid and accurate signal detection. The advancements in Artificial Intelligence has resolved such issues by integrating advanced analytics, natural language processing and machine learning algorithms to enhance PV processes. This ability of AI to automate adverse event detection, mine unstructured data from electronic health records and predict potential drug risks with accuracy has redefined the scope of PV.
The New Frontier in Drug Safety
In an era where medicine is advancing at an unprecedented pace, ensuring the safety of pharmaceutical products has become more challenging than ever. The sheer volume of new drugs, complex formulations, and global distribution networks has made traditional pharmacovigilance methods increasingly difficult to manage. For decades, drug safety monitoring relied heavily on spontaneous adverse event reporting, manual data entry, and retrospective analysis—processes that, while valuable, are often slow, reactive, and prone to human error. But what if we could predict potential safety concerns before they become widespread health threats? This is where artificial intelligence (AI) steps in, transforming pharmacovigilance from a reactive practice into a proactive, data-driven discipline.
AI is not just enhancing pharmacovigilance—it is redefining it. With advanced machine learning algorithms, deep learning models, and natural language processing (NLP) capabilities, AI can rapidly analyze vast amounts of structured and unstructured data from multiple sources, including electronic health records, scientific literature, patient forums, and even social media discussions. By detecting subtle safety signals that might go unnoticed through conventional methods, AI is accelerating the identification of adverse drug reactions (ADRs) and providing regulatory agencies and pharmaceutical companies with critical insights in real time.
Global regulatory bodies such as the FDA, EMA, and MHRA have already begun integrating AI-driven tools into their drug safety monitoring frameworks. Pharma giants are leveraging AI for automated case processing, predictive risk assessments, and real-world evidence analysis, leading to faster decision-making and improved patient outcomes. This technological revolution is not just about efficiency—it’s about safeguarding lives by minimizing the risks associated with pharmaceuticals. As we enter a new age of intelligent drug safety surveillance, one thing is clear: AI is no longer a futuristic concept in pharmacovigilance. It is here, it is evolving, and it is fundamentally reshaping how we monitor, manage, and mitigate drug-related risks. The question is not whether AI will transform pharmacovigilance, but rather how far its capabilities will go in shaping a safer and smarter future for global healthcare.
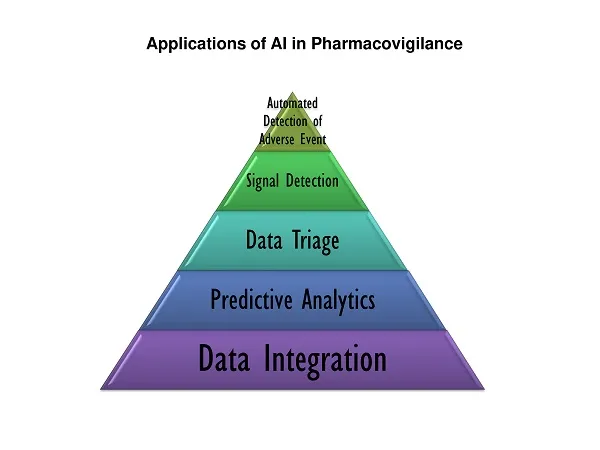
Understanding the Role of AI in Pharmacovigilance
AI is revolutionizing pharmacovigilance by enhancing the detection, analysis, and reporting of adverse drug reactions (ADRs). Its capabilities range from automating case processing to identifying safety signals from vast datasets. Here’s how AI is making an impact across key PV domains:
- Automated Case Processing: AI-powered tools can rapidly extract relevant data from electronic health records (EHRs), patient forums, and scientific literature, reducing the manual burden on pharmacovigilance professionals. Natural Language Processing (NLP) and machine learning (ML) facilitate structured case reporting with higher accuracy and consistency.
Pharmaceutical companies are increasingly adopting AI-based tools to streamline adverse event reporting. For instance, algorithms developed by companies like IBM Watson Health analyze patient narratives from electronic health records to identify and report potential adverse drug reactions, reducing reporting delays. Social media platforms, a goldmine of patient-reported outcomes, are also being leveraged. AI tools like sentiment analysis and topic modeling monitor discussions on platforms such as Twitter, Facebook, and patient forums to identify emerging safety issues.
- Advanced Signal Detection: Traditional signal detection relies on spontaneous reporting databases, but AI enhances this process by integrating data from multiple sources, including social media, wearable devices, and real-world evidence. Machine learning models identify previously unnoticed ADR patterns, enabling early intervention.
Another significant advancement is the use of Natural Language Processing (NLP), which helps extract valuable insights from unstructured text sources such as medical literature, online discussions, and patient reviews. Crucial drug safety information is often buried in research papers, physician notes, and informal patient discussions on platforms like Twitter and Reddit. NLP-powered AI can analyze and interpret these vast amounts of data, identifying ADRs that may not be captured through traditional reporting systems. Additionally, NLP can translate informal language and slang used by patients when describing their symptoms, making the monitoring process more inclusive and accurate.
AI-powered systems can now scan electronic health records, social media platforms, and patient forums to detect ADRs in real time. This automation reduces human effort and allows regulatory bodies to respond faster to potential safety concerns. For instance, organizations like the FDA and EMA are integrating AI into their surveillance systems to accelerate safety signal detection and ensure quicker regulatory action.
- Predictive Pharmacovigilance:
Beyond detecting ADRs, AI is also enhancing predictive pharmacovigilance. Machine learning models can analyze large datasets to identify patterns and correlations that help predict potential adverse reactions for both new and existing drugs. This predictive capability enables pharmaceutical companies and regulators to identify high-risk drugs early in development, potentially preventing harmful effects before a drug reaches the market. Researchers are now leveraging AI to predict rare ADRs using real-world patient data, an advancement that was nearly impossible with traditional methods.
AI-driven predictive analytics can anticipate potential safety concerns even before large-scale clinical data is available. By analyzing historical ADR data and genetic predispositions, AI models help forecast which patient populations might be at higher risk for specific drug reactions.
- Real-Time Data Surveillance: Continuous monitoring of drug safety through AI-driven platforms ensures real-time surveillance, enabling quicker response times to emerging safety signals. AI-enhanced dashboards assist regulatory bodies and pharmaceutical companies in making informed decisions with up-to-date insights.
- Automated Literature Review & Regulatory Reporting: AI expedites the literature review process by scanning millions of journal articles, identifying relevant findings, and generating structured summaries. It also streamlines compliance reporting by aligning case reports with regulatory guidelines set by agencies like the FDA and EMA.
AI is also improving pharmacovigilance through interactive AI-powered chatbots. These virtual assistants provide real-time drug safety information to healthcare professionals and patients, answering queries about potential side effects and guiding users through the process of reporting ADRs. Some pharmaceutical companies have even launched AI-driven virtual assistants that can interpret patient symptoms and detect potential adverse effects, making drug safety monitoring more proactive and patient-centric.
Despite its many advantages, AI in pharmacovigilance requires robust safety guardrails to ensure accuracy and compliance with regulatory standards. AI models, while powerful, are not infallible and need frameworks that detect incorrect data, prevent bias, and alert users about potential AI errors. Leading regulatory agencies, including the FDA, are actively developing ethical AI guidelines to maintain transparency and accountability in AI-powered pharmacovigilance. Rather than replacing human experts, AI is being designed to support and enhance decision-making, ensuring that drug safety assessments remain reliable and evidence-based.
The Impact of AI on Patient Safety and Regulatory Compliance
The integration of AI into pharmacovigilance is not just about operational efficiency—it has profound implications for patient safety and regulatory compliance. AI-driven systems minimize underreporting and misclassification of ADRs by capturing signals from diverse and unconventional data sources. This enhances post-marketing surveillance and ensures that emerging risks are identified before they escalate into public health concerns.
Moreover, AI optimizes regulatory reporting by automating submission workflows and ensuring compliance with stringent global safety standards. Regulatory agencies are now exploring AI-assisted tools for processing Individual Case Safety Reports (ICSRs) and Periodic Benefit-Risk Evaluation Reports (PBRERs), reducing delays in safety assessments.
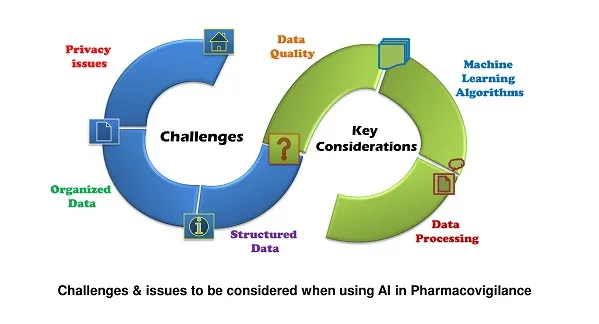
Challenges in AI-Driven Pharmacovigilance
Despite its promise, the adoption of AI in pharmacovigilance comes with challenges:
- Data Quality and Bias: AI models are only as good as the data they are trained on. Incomplete or biased datasets can lead to incorrect safety signals, necessitating rigorous data curation and validation. The dependency on training data is seen in the development and deployment of machine learning algorithms that enable numerous artificial intelligence programs. Complex algorithms require vast amounts of data, and in many circumstances, there is no (or insufficient) training data available. In other circumstances, the training data may not adequately represent the problem to be solved, and the resulting algorithm may be similarly misaligned. Machine learning algorithms may potentially replicate previous systematic flaws seen in training data. When the algorithms themselves are difficult to understand, it is essential that the training data on which they are optimised be plainly disclosed.
- Interpretability of AI Decisions: Regulatory authorities demand transparency in safety assessments. AI’s "black-box" nature remains a concern, and efforts are being made to develop explainable AI (XAI) models that provide interpretable results. Lack of transparency offers particular challenges for intelligence augmentation, as people must communicate effectively with computer algorithms and consider their recommendations in their own decision-making. Evaluation of such hybrid systems also provides distinct issues due to the heterogeneity among human specialists and the way they communicate with computers.
- Regulatory Acceptance: While AI is making strides in PV, regulatory frameworks are still evolving. Pharmaceutical companies must navigate compliance challenges while adopting AI-driven solutions.
- Integration with Existing Systems: Many pharma companies operate on legacy systems that may not be AI-compatible. A seamless transition to AI-powered pharmacovigilance requires strategic digital transformation initiatives. The ability of machine learning algorithms to evolve over time and acquire knowledge from new experiences and data is a key strength and requirement for their continuous relevance and accuracy in changing contexts. Simultaneously, continuous change makes auditing and inspection difficult. Special procedures may need to be made to ensure that prior results and predictions can be replicated and understood. For instance, if a relevant signal was not detected because adverse events were incorrectly encoded by a machine learning algorithm, we must be able to determine which version of the algorithm was in use at the time the incorrect encodings occurred.
- The Future of AI in Pharmacovigilance
The trajectory of AI in pharmacovigilance is poised for further growth. The incorporation of big data analytics, federated learning, and blockchain will enhance data security, interoperability, and global collaboration. AI-powered chatbots and virtual assistants will facilitate real-time ADR reporting by engaging with patients and healthcare professionals seamlessly.
Furthermore, the future will see greater emphasis on AI-human collaboration, where AI handles data-heavy tasks while human experts focus on clinical judgment and decision-making. By bridging technological advancements with regulatory adaptations, AI will redefine pharmacovigilance as a proactive, patient-centric ecosystem.
Conclusion: A Smarter, Safer Future
The infusion of AI into pharmacovigilance marks a paradigm shift from traditional reactive drug safety monitoring to a more intelligent, predictive, and real-time approach. As AI continues to evolve, its ability to process complex datasets, identify safety signals, and enhance regulatory compliance will play a pivotal role in ensuring safer pharmaceuticals for global populations. While challenges remain, the fusion of AI with human expertise is set to unlock unprecedented advancements in pharmacovigilance, ushering in a new era of patient safety and regulatory excellence.
References
- Yu KH, Beam AL, Kohane IS. Artificial intelligence in healthcare. Nat Biomed Eng 2018;2:719‑31.
- Basile AO, Yahi A, Tatonetti NP. Artificial intelligence for drug toxicity and safety. Trends Pharmacol Sci 2019;40:624‑35.
- Murali K, Kaur S, Prakash A, Medhi B. Artificial intelligence in pharmacovigilance: Practical utility. Indian J Pharmacol 2019;51:373-6.
- CIOMS Concept Paper – Artificial Intelligence in Pharmacovigilance, February 2, 2022.
- Ball R, Dal Pan G. "Artificial Intelligence" for pharmacovigilance: ready for prime time? Drug Saf 2022;45:429–38.
- Bate A, Luo Y. Artificial intelligence and machine learning for safe medicines. Drug Saf 2022;45:403–5.
- Zhao Y, Yu Y, Wang H, Li Y, Deng Y, Jiang G, Luo Y. Machine learning in causal inference: application in pharmacovigilance. Drug Saf 2022;45:459–76.
- Kompa B, Hakim JB, Palepu A, Kompa KG, Smith M, Bain PA, Woloszynek S, Painter JL, Bate A, Beam AL. Artificial intelligence based on machine learning in pharmacovigilance: a scoping review. Drug Saf 2022;45:477–91.











