Antibiotic Resistance 101: What Everyone Needs to Know About Superbugs
Debi Jones, Editorial Team, Pharma Focus America
The two threats to global health are bacterial resistance because bacteria populations can modify themselves to become resistance to the essential medicines needed to manage infections. It defines the reasons for resistance including misuse, agriculture, bad hygiene, and travel and provides prevention ideas including right use of antibiotics, washing, vaccination and research to fight superbugs.

Introduction:
Misuse poses a security threat that threatens human life, and antibiotic resistance is ranked very high as a health risk in the world. These are formed when bacteria tend to develop mechanisms of resistance against drugs that are used for clearing the bacteria. As such, when it comes to ordinary illnesses and diseases, which can, therefore, positively respond to prescribe medication, and tend to be regarded as normal day to day diseases, they cannot be treated rightly or are untreatable altogether.
It will be desirable that every person acquired the most minimal knowledge concerning what antibiotic resistance is, how it occurred, how it influenced health, and how its manifestation can be prevented. The issues we will discuss in this article include for example; what are superbugs? Why is antibiotic resistance unavoidable? And; how can you stop it?
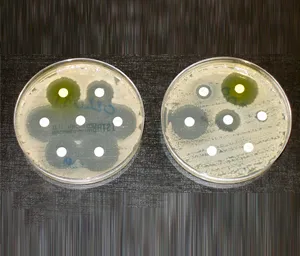
What Are Superbugs?
It is only a mixture of bacteria that cannot be erased by a number of forms of antibiotics; thus it is hard to get rid of. Every time doctors prescribe antibiotics, they anticipate that these will clear out the bacteria that is causing an infection. Yet there is always a few, which can overcome the effects and thus form super hardy organisms known as superbugs. Such resistant bacteria prolong the hospital duration, expensive to treat and are likely to lead to the death of the patient.
Popular superbugs include: Among the most common hospital acquired infection resistant organisms, they include; Methicillin-resistant Staphylococcus aureus (MRSA), Vancomycin-resistant Enterococcus (VRE) and multi-drug resistant Escherichia coli (MDR E.Coli). Infections like these are dangerous in hospitals because the patient could have a compromised immune system or the patient could be having an open wound.
Antibiotic resistance is a simple developmental effect that occurs within bacteria when in contact with antibiotics; these organisms grow in such environments. Several factors contribute to this phenomenon:
How Does Antibiotic Resistance Happen?
Antibiotic resistance on its part can be defined as a developmental response of these bacteria to antibiotics – these organisms grow in these environments. Several factors contribute to this phenomenon:
- Overuse and Misuse of Antibiotics: Antibiotic misuse and the use of antibiotics still stands as the main cause for antibiotic resistances. If people take tablets in the wrong proportion or use antibiotics to cure ailments such as the flu and the common cold, the bacteria becomes resistant.
- Agricultural Practices: They can also be used in food industry in order to help grow the healthy animal. This practice can also create resistant bacteria in livestock that may then be ingested but the food chain by humans.
- Poor Infection Control: In health care delivery, poor infection control measures expose patients to more resistant bacterium. For instance, if health care givers in a hospital are careless to push for cleanliness of their hands or surgical knives, among other apparatus’ then it is most probable that superbugs will easily spread across many patients.
- Global Travel and Trade: Antibiotic bacteria can from one country to another in the blink of an eye, as more individuals commute, and more products transported from one place to another. A person carrying superbugs in one country can transmit it to a next country making it a global menace.
The Impact of Antibiotic Resistance
Antibiotic resistance: A critical appraisal of threat perceptions. Serialization and type of antibiotic arms: Threats to public health. This complicates treatment strategies and results in longer stay in hospital and more rigorous care. Infections with such bacteria can also be more deadly, thus leading to an application of other treatments which are usually more toxic.
The Centers for Disease Control and Prevention (CDC) estimates that at least 2.8 million people in the United States get infected with antibiotic-resistant bacteria annually and result in more than 35,000 deaths. The ASBs also showed high financial impacts as would be evidenced by increased health costs and productivity losses from longer disease and death.
Prevention and Control
While the threat of antibiotic resistance is serious, there are steps we can all take to help combat the problem:
- Use Antibiotics Responsibly: Regardless of the completion of the pills, or no more signs and symptoms to show, should not take lesser or more of the antibiotic than the doctor recommended. They should not be taken or to be administered to others or be used in treating a different disease from what is being treated. This means that is very important to always complete a course of antibiotics even if the last dose of a specific antibiotic makes one uncomfortable.
- Avoid Unnecessary Antibiotics: It is always important to remember that antibiotic medicines can only cause harm to viral infections only. In the case your doctor has given you antibiotics it needs to be that they are necessary for your circumstance. See your healthcare provider and discuss with him/her if you have questions over the use of antibiotics.
- Practice Good Hygiene: It is important to know that washing the hands with soap and water can reduce transmission of infective health issues by up to half. Sanitizers, especially in identified health care centers, should also be used. It also minimizes the possibility of contacting infections on the open wounds one may develop at some point in life.
- Vaccination: Admittedly, the effectiveness of vaccines has been acknowledged in a variety of infections, the application of which reduces the need for antibiotics. Vaccination is cheap and acts as a shield against diseases you are prone to get and this affect you and people around you.
- Support Responsible Agriculture: Promote the use of farms with a proper usage of antibiotics and act as a customer for these farms. Buy only antibiotic-free products and whenever possible, go for meats and dairy products that have been produced without the administration of antibiotics intended for growth.
- Promote Research and Development: Promote policies that seem to favor new antibiotic discovery and seek for other means of curing the diseases. This is a challenge the pharmaceutical industry struggles with, in formulating new antibiotics since the costs are high and yet the returns are low. Increasing funding towards research for antibiotics will require encouraging policy which enables new treatment.
What Is Being Done Globally?
It is laudable that governments, organizations and global healthcare systems are beginning to appreciate the need to fight antibiotic resistance more. Programs like the World Health Organization's (WHO) Global Action Plan on Antimicrobial Resistance are usually established to address such threat. Some of these efforts include; improvement in surveillance of antibiotic-resistant infections, strengthening of that of infection prevention and control, and appropriate utilization of antibiotics.
In United States, the CDC has begun with Antibiotic Resistance Solutions Initiative that is the organization has endeavored to know the trends in relation to antibiotic resistance, improve the utilization of antibiotics as well as improve the consciousness among the health care practitioners and the general society population.
The Role of Healthcare Providers
Firstly, healthcare providers are acknowledged as one of the stakeholders in the battle against antibiotic resistance. They are required to ensure that antibiotics are prescribed appropriately, they are required to educate their clients on the improper use of antibiotic drugs. Moreover, the providers need to understand the local antibiotic stewardship to make appropriate treatment choices regarding antibiotic use. Infection control practice in healthcare facilities are also important as well. This can be proper equipment cleaning and disposal, hand washing and good patient isolation for cases of stubborn illnesses.
Conclusion
Antibiotic resistance is multi factorial and rising issue that is considered to be a major threat to human health. It is important that everyone know about the factors causing the antibiotic resistance and the effects that arise from it.
Amidst the increasing cases of superbugs, decreased cases can be achieved if people use antibiotics bearing in mind their effects as well as observing hygiene and advocating for farmers to use best practices in animal farming and research and awareness creation. If used strategically, antibiotics will be around for future generations to use and thus save our future health from consulting. To overcome the regulatory difficulty of antibiotic resistance, everyone, and especially healthcare providers and communities, must join forces.